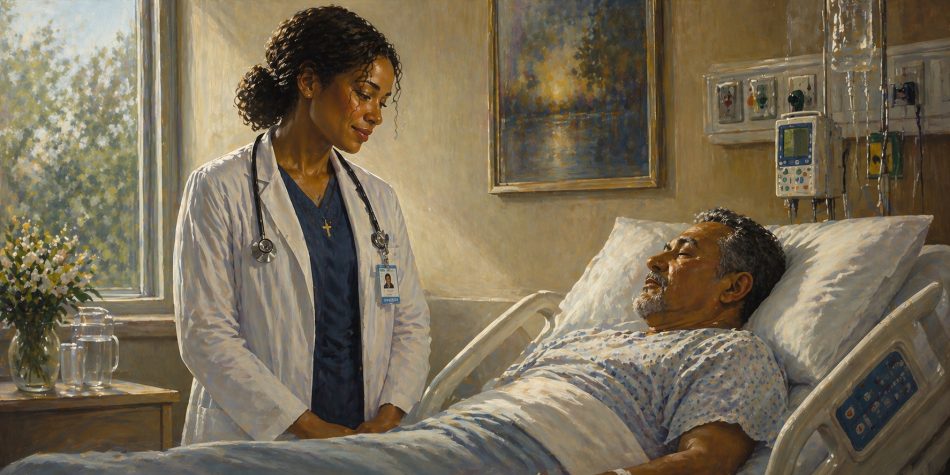Would you prefer to be treated by a physician who follows her conscience or one who does not?
Most, if not all, of us would prefer a physician who follows her conscience. But the pressure is increasing for Christian health care professionals to choose between their careers and consciences.
Whether it is a medical student being forced to train to perform abortions, a pharmacist being asked to fill lethal prescriptions for assisted suicide, or a physician asked to administer anesthesia to a minor patient undergoing a sex-rejecting procedure, many Christian health care professionals are leaving the field of medicine, taking with them countless years of training.
This leaves fewer ethical, morally grounded health care professionals—a trend that is dangerous for both health care systems and patients. With the growing departure of ethical health care professionals from the field of medicine, and the field of medicine increasingly untethered from ethics, conscience protections are necessary to sustain the participation of faith-based health care professionals.
The Tradition of Hippocratic Medicine
Our culture is rapidly shifting away from the longstanding foundation of Western health care. For those who espouse the Hippocratic tradition—to not kill the patient, to not give a pregnant woman an abortifacient, and to do no harm—there remains a real threat of being made complicit in actions that they deem evil. Sometimes it may not be possible for health care professionals to separate themselves from these situations.
Unfortunately, ideologies that reject the Hippocratic tradition have become pervasive. Society has elevated autonomy as a primary good: what the patient wants is presumed best, regardless of whether it harms the patient. There is little pushback against the ideas that prenatal life is inferior or that we should hasten death for those who have given up on life. This same rejection of the Hippocratic tradition is evident in transgender medical interventions, where subjective desires are allowed to override biological sex, resulting in the destruction of healthy, God-given bodies. Furthermore, the structure of our modern health system, like our broader culture, often pursues efficiency for its own sake, subjugating patient well-being.
Unfortunately, ideologies that reject the Hippocratic tradition have become pervasive.
Serving on the advocacy team of the Christian Medical & Dental Associations (CMDA), the nation’s largest faith-based professional health care organization, we help to advance policies at the state and federal levels to protect the vulnerable—the unborn, those at the end of life, and everyone in between. We also advocate for the conscience protections and religious freedom of health care professionals, protections that are especially vital for those seeking to uphold Hippocratic traditions amid contemporary bioethical issues.
Conscience in the Clinic
Many Christian health care professionals are pressured to capitulate to patient whims, bureaucratic mandates, profit-first business models, academic requirements, or laws that challenge their moral compasses, driving them out of the field. Patient autonomy, in particular, has become a key component of today’s health care. But not every “treatment” a patient seeks leads to human flourishing. Some patients seek providers who will serve as personal vending machines, dispensing whatever is requested, regardless of its ethical or medical soundness. This dynamic subverts the role of the health care professional, who is supposed to exercise expertise in providing ethical, scientifically backed care to the patient—not simply be the patient’s puppet.
Our ethics, faith, and values should not be compartmentalized within our places of worship. They should be embodied within us wherever we go, including our workplaces. Health care professionals and students who follow Christ carry within them the gospel of truth that transforms patient care. They see both the immediate suffering and the eternal significance of the person. They see the patient as a person deserving compassionate care, whereas in the profit-first, secular care setting, the tendency is to see the patient as a problem to be solved with a checklist. Christian health care professionals also see and treat their patients as image bearers of God, worthy of treatment in accordance with the highest ethical standards.
The Protections Needed
So when should health care professionals be able to say “no” to requests that would violate their conscience?
For one, they must have the right to refuse to participate in specific procedures or treatments that conflict with their professional conscience, such as treating the patient contrary to the Hippocratic standard. This includes being protected from having to perform or assist with abortions or help a patient end her life through assisted suicide.
They must say “no” when forced participation in a procedure would result in moral injury to the professional.
Relatedly, they must say “no” when forced participation in a procedure would result in moral injury to the professional. Every month, CMDA receives inquiries from students, residents, fellows, and practicing health care professionals seeking assistance after being asked to violate their consciences by providing a specific service. Some health care professionals simply quit or move to another state to avoid violating their consciences. Others have been fired, often resulting in lawsuits.
Ultimately, no health care professional should be forced to choose between their life’s vocational calling and their ethical, moral, or religious values. The Christian health care professional enters the profession to serve patients and provide care according to the highest ethical standards—qualities that should be promoted, not punished.
Legislative Protections
Legislation is vital to securing the conscience rights of health care professionals. Codifying conscience protections helps the health care field to retain ethical professionals who might otherwise leave or relocate to more conscience-protective jurisdictions.
Supporting the moral integrity of our health care profession is in everyone’s best interest. Whether they are medical students or physicians with decades of experience, CMDA members report that they are often mandated to refer for procedures that violate their consciences, becoming cash registers rather than caring health care professionals. Some of them have been discriminated against in the workplace for their beliefs, or they know other health care professionals who have faced discrimination for declining to participate in activities or medical procedures to which they had moral or religious objections. This is occurring to such a degree in multiple states and specialties of practice that some of our members are considering walking away from the field of medicine altogether rather than be compelled to violate their consciences.
Our 2019 survey of 1,732 health care professionals revealed the depth of this crisis:
- 76 percent of those surveyed in certain specialties noticed or had experienced increased pressure to compromise their moral, ethical, or religious beliefs in their practices.
- 33 percent of health care professionals had been pressured, forced, or punished to refer a patient for a procedure to which they had moral, ethical, or religious objections.
- 91 percent of respondents reported they “would rather stop practicing medicine altogether than be forced to violate [their] conscience.”
We applaud the passage of health care conscience protection bills in state legislatures and in the U.S. Congress. Before the 2026 legislative session, nine states (Arkansas, Florida, Idaho, Illinois, Mississippi, Montana, Ohio, South Carolina and Tennessee) had passed health care conscience laws known as the Medical Ethics Defense (MED) Act or similar legislation. In the 2026 legislative session, similar bills were considered in Iowa, Kentucky, Nebraska, New Hampshire, Oklahoma, Rhode Island, South Dakota, and Utah. As of this writing, the MED Act has passed in the Iowa and Utah legislatures.
These bills, while varying by state, aim to protect the freedom of health care professionals to practice according to their consciences. They allow health care professionals to decline to perform procedures that violate their ethical standards and religious beliefs. And they shield health care professionals from losing their jobs or facing criminal charges for practicing conscientiously.
These bills are procedure-specific; for example, they provide statutory protection for health care professionals who decline to perform, assist in, or train for abortions, as well as those who refuse to refer for or provide lethal prescriptions for assisted suicide. The bills do not allow discrimination against individual patients. Health care professionals cannot refuse to care for a patient. In fact, these laws are intended to protect those who seek to provide only the best care for their patients by avoiding the infliction of harm to patients.
These bills are necessary to address the current lack of federal enforcement. Moreover, while some states have outlawed certain procedures, technology is advancing at such a pace that new unethical services will inevitably arise. We need protections to safeguard the practice of ethical medicine against challenges we have yet to encounter.
At the federal level, protections currently exist through the Church, Coats-Snowe, and Weldon Amendments.
- The Church Amendment ensures health care professionals and hospitals are not required to assist in abortions or sterilizations that violate their moral or religious beliefs. It is one of the most important federal protections on the basis of religious beliefs or moral convictions.
- The Coats-Snowe Amendment protects physicians and health care entities from being forced to perform, refer for, or make arrangements to refer for abortions. Crucially, it applies to any government entity that receives federal financial assistance, so students and residents at federally funded medical institutions cannot be forced to be involved in abortions.
- The Weldon Amendment prohibits federal agencies and programs, and state and local governments, from discriminating against any health care entity, professional, or insurance plan for refusing to provide, pay for, provide coverage of, or refer for abortions.
While not yet law, the Conscience Protections for Medical Residents Act would provide another essential federal protection. By replacing the current abortion training “opt-out” system—which often subjects residents who opt out to discrimination—with an “opt-in-only” system, the bill would better protect the rights of residents with conscientious objections.
Although existing federal laws provide strong protections, their efficacy depends on enforcement, and that is a problem. Each administration at the Department of Health and Human Services prioritizes different protections, often redefining the concept of conscience to align with its larger policy goals. Consequently, states have been stepping up efforts with their respective MED Act legislation to provide the safeguards that the federal government fails to guarantee. These persistent gaps make bills such as the Conscience Protections for Medical Residents Act a critical priority for our mission.
But What About …
Some are concerned that if physicians have conscience protections, patients will be unable to receive care.
The CMDA agrees that if a procedure is legal, a patient has the right to seek it out. But a patient does not have the right to conscript a specific, unwilling physician into violating their deeply held beliefs to provide it.
Conscience freedom laws are procedure-based, not patient- or person-based. Physicians are to provide the best medical treatment in any given situation. Professionals with conscience objections to certain courses of treatment will refuse anti-Hippocratic treatment for any patient requesting it. They do not discriminate against individuals; they simply choose to not engage in certain procedures that they believe are harmful to patients.
Notably, the medical interventions that prompt these conscience-based refusals are elective in nature. If a patient believes a treatment that a conscientious provider will not provide is the best course of action, the patient can seek that treatment elsewhere.
Health care providers must not be mere machines deployed by their employers in the service of every desire of their patients, according to ideologies that are constantly in flux. A health care professional must have the ability to refuse what they know is wrong.
A Duty to the Truth
What do we lose when we don’t protect conscience?
Most certainly, we lose the trust that is so essential in a health care system. Violation of conscience creates distrust. Because trust is essential in a patient-health care professional relationship, we must respect the fundamental ethical right and freedom of clinicians to follow their consciences and to resist pressures that would undermine their integrity.
For example, if the right of professionals to conscientiously abstain is not protected, what prevents health systems from requiring their employees to provide services that are good for the system’s bottom line but that harm the patient’s health and flourishing?
The Christian church community and the health care professions can work in tandem.
If health professionals cannot conscientiously abstain, how can we be sure we won’t end up committing the atrocities carried out by many physicians at the behest of the state as recently as the 20th century? We should recall that lobotomies were once widely used in just the last century, and now they would be considered malpractice.
Conscience protections also allow for pushback against today’s popular consensus that could very well change tomorrow. (For example, look at the Cass Review, an independent report commissioned by the U.K. that concluded the evidence for treating minors with gender dysphoria with puberty blockers and sex hormones was “remarkably weak”). These are protections for the patient as much as they are for the physician. Conscience protections allow for physicians to remain genuine expert professionals rather than becoming vending machines that cater to their patients’ every desire.
If elective abortion or assisted suicide is more cost-effective for hospitals than treating a difficult diagnosis, ensuring your physician chooses the highest standards of care over the path of least resistance is vital. These are the kinds of professionals we want to retain.
When we don’t protect conscience, we also lose out on many professionals whose conscience drives their desire to emulate the health care and Christlike role of healer. We miss the virtue these physicians cultivate when they can live by their highest ethical standards.
Christianity and Health Care Working Together
The Christian church community and the health care professions can work in tandem. Those in the health care profession can help the church to understand the truth about complex bioethical issues, while the church can serve as the guardrails and remind those in health care to be compassionate and courageous without compromise. As Dr. Brick Lantz, CMDA Vice President of Advocacy and Bioethics notes, “It is a two-way street, as we in health care also need the church’s help to encourage and empower us to do good.”
In the book “How Now Shall We Live,” Charles Colson and Nancy Pearcey argue that the world is divided by two worldviews: secular and biblical. Bridging the gap between them begins by acknowledging the Fall and the need for transformation by the Holy Spirit. As Colson writes, “The secular view has been tried and found wanting, and its failure opens a wonderful opportunity for Christians to make a case for a biblical worldview of human nature and community.”
We do not want a gospel of accommodation that allows a secular world to reject God’s terms and His design. The consequences of such accommodation and departure from the truth are already producing devastating effects on men, women, children, families, and society, not to mention their pervasive distortion of health care. The gospel and the church are the solution to stem this decay and distortion by protecting what God says is good.
As Nicole wrote previously in “The Right to Believe: The New Struggle for Religious Liberty in America,”:
America heralds itself as a free society committed to not impede the free exercise of religion per our First Amendment rights. … However, those who show restraint from engaging in things that would be considered “progress,” or “compassionate” but rather they are evil, we are looked upon with disdain. It seems that America’s pursuit of progress is to liberate those who wish to trespass the moral boundary lines that our holy God has established.
We need to protect the conscience freedoms of health care professionals who object to participating in procedures under the guise of “autonomy” and “progress” that disregard our inherent dignity. By protecting conscience and religious freedoms in health care, we are protecting health care professionals and patients from being subjected to the “enhancements” that a secular worldview may contemplate. Patients deserve health care professionals who are conscientious and humbled by the fact that we are all created in the image of God. Conscience should always be motivated by a love for God and our neighbor. By demonstrating a better way, conscientious refusal enables the Christian health care professional to overcome evil with good (Romans 12:21).